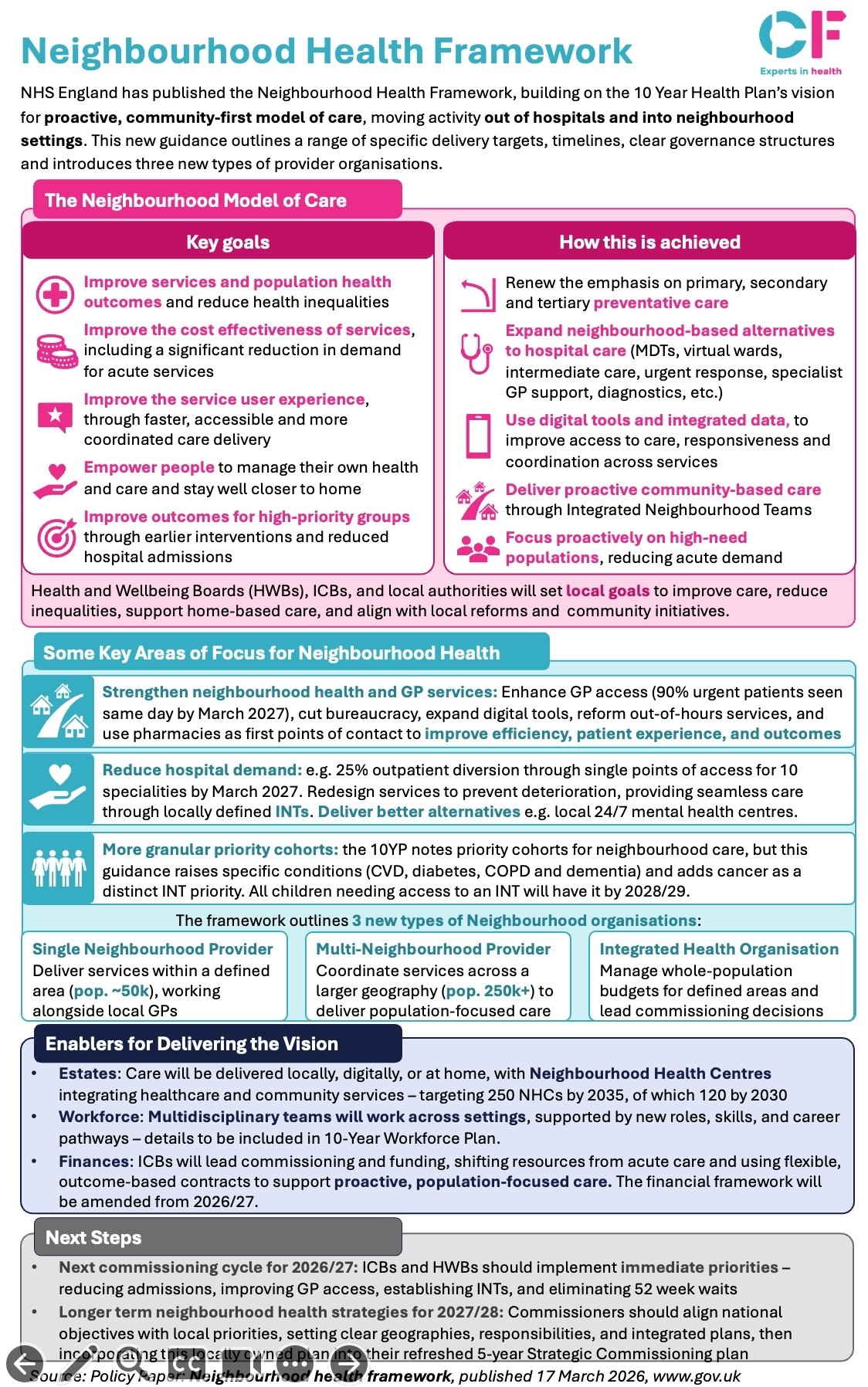
NHS England has published the Neighbourhood Health Framework, building on the 10 Year Health Plan’s vision for a proactive, community-first model of care, moving activity out of hospitals and into neighbourhood settings. This new guidance outlines a range of specific delivery targets, timelines, clear governance structures and introduces three new types of provider organisations.The Neighbourhood Model of Care outlines five key goals:
- Improve services and population health outcomes, reducing health inequalities
- Improve the cost effectiveness of services, including a significant reduction in demand for acute services
- Improve the service user experience, through faster, accessible and more coordinated care delivery
- Empower people to manage their own health and care and stay well closer to home
- Improve outcomes for high-priority groups through earlier interventions and reduced hospital admissions
These goals will be achieved by renewing the emphasis on primary, secondary and tertiary preventative care; expanding neighbourhood-based alternatives to hospital care (MDTs, virtual wards, intermediate care, urgent response, specialist GP support, diagnostics, etc.); using digital tools and integrated data to improve access, responsiveness and coordination across services; delivering proactive community-based care through Integrated Neighbourhood Teams; and focusing proactively on high-need populations to reduce acute demand.
Health and Wellbeing Boards (HWBs), ICBs, and local authorities will set local goals to improve care, reduce inequalities, support home-based care, and align with local reforms and community initiatives.
Some key areas of focus for Neighbourhood Health include:
See the full snapshot below:
The framework outlines 3 new types of Neighbourhood organisations:
- Single Neighbourhood Provider – Deliver services within a defined area (pop. ~50k), working alongside local GPs
- Multi-Neighbourhood Provider – Coordinate services across a larger geography (pop. 250k+) to deliver population-focused care
- Integrated Health Organisation – Manage whole-population budgets for defined areas and lead commissioning decisions
The key enablers for delivering the vision are:
- Estates: Care will be delivered locally, digitally, or at home, with Neighbourhood Health Centres integrating healthcare and community services – targeting 250 NHCs by 2035, of which 120 by 2030
- Workforce: Multidisciplinary teams will work across settings, supported by new roles, skills, and career pathways – details to be included in the 10-Year Workforce Plan
- Finances: ICBs will lead commissioning and funding, shifting resources from acute care and using flexible, outcome-based contracts to support proactive, population-focused care. The financial framework will be amended from 2026/27
The next steps for the commissioning cycle of 2026/27 see ICBs and HWBs implementing immediate priorities – reducing admissions, improving GP access, establishing INTs, and eliminating 52 week waits.
Longer-term neighbourhood health strategies for 2027/28 should see commissioners aligning national objectives with local priorities, setting clear geographies, responsibilities, and integrated plans, then incorporating this locally owned plan into their refreshed 5-year Strategic Commissioning plan.
Find the full framework here.